The Revenue Cycle Blog
Filter By
- ABA Therapy Billing
- AI in Medical Billing
- AI in Revenue Cycle
- ASC Billing Services
- Accounts Receivable Management
- Accounts Receivable Mangement
- Allergy and Immunology Billing Services
- Anesthesia Billing Services
- Back Office Revenue Cycle
- Bariatric Surgery Billing
- Billing For Physician Practice and Medical Groups
- Billing for Physician Practices and Medical Groups
- Blog
- COVID-19 Billing
- CPT Codes
- Cardiology Billing Services
- Charge Capture Services
- Charge Entry - Medical Billing
- Charge Entry Services
- Clinical Documentation Improvement - CDI
- Clinical Documentation Integrity
- Company News
- Credit Balance Services
- DME Billing Services
- Denial Code CO-97
- Denial Management - Medical Billing
- Dermatology Billing Services
- E&M
- Electronic Health Records
- Eligibility and Benefits Verification Services
- Emergency Department Billing Services
- FAQs
- Family Practice Billing Services
- G Code
- Gastroenterology Billing Services
- General Surgery Billing Services
- HCC Coding
- HCC Coding Services
- HCPCS
- Healthcare Collections
- Hospitals
- Internal Medicine Billing Services
- Medical Billing Company
- Medical Billing Services
- Medical Billing Services in California
- Medical Billing Services in Texas
- Medical Claim Submission
- Medical Coding Services
- Mental Health Billing Services
- Mental health Billing Services
ICD 10 Ocular Trauma Coding: Documentation & Shortcuts
ICD 10 ocular trauma coding requires proper documentation, correct injury classification, and accurate code selection for timely billing. This blog covers documentation requirements, coding workflow, and shortcuts used to identify ICD-10 ocular trauma codes efficiently, along with a quick reference table to support faster coding.
Optometry Billing and Coding Cheat Sheet for Hospital (2026)
Hospital optometry billing in 2026 requires proper coding, accurate documentation, and compliance with medical billing rules. This Optometry Billing and Coding Cheat Sheet covers E/M codes, ICD-10, modifiers, and billing guidelines to help reduce denials and improve reimbursement in hospital settings.
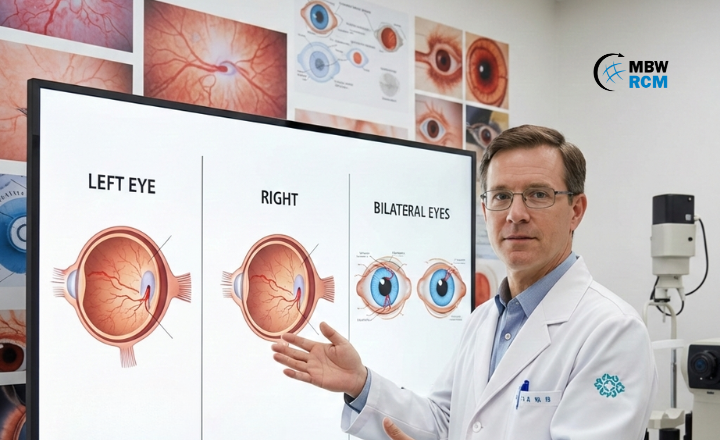
Retinal Detachment ICD 10 Code for Left, Right & Bilateral Eyes
Retinal Detachment ICD 10 Code for Left, Right & Bilateral Eyes explains diagnosis code selection based on detachment type, laterality, and clinical documentation. This blog covers commonly used ICD-10 codes, eye-specific coding differences, and key documentation points for retinal detachment diagnosis and ophthalmology billing.
Ocular Trauma ICD-10: Do’s & Don’ts in Medical Coding
Ocular trauma ICD-10 coding requires careful attention to injury type, laterality, and treatment phase. This blog covers essential Do’s and Don’ts to help reduce coding errors and support correct eye injury code selection in real-world scenarios.
Top 10 Ophthalmology Billing Companies in USA
Explore the top ophthalmology billing companies in the USA and how specialty-focused billing partners help reduce denials, improve coding accuracy, and strengthen revenue performance for cataract, retina, and glaucoma services.
Ophthalmology Billing and Coding for Retina, Cataract and Glaucoma Services
Ophthalmology billing and coding for retina, cataract, and glaucoma services demand careful CPT selection, modifier use, and documentation. This guide outlines key requirements and best practices to help practices reduce denials and maintain consistent reimbursement.
Case Study: Resolving Ophthalmology NPI/TIN Mismatches to Prevent Out-of-Network Losses
An ophthalmology practice in New York faced major reimbursement issues when incorrect NPI/TIN setup caused in-network claims to process as out-of-network. MBW RCM identified the mismatch, corrected the provider configuration, and helped the practice prevent further revenue loss.
Case Study: Eliminating $151,695 in Coding-Related Denials for a South Dakota Ophthalmology Practice
A South Dakota ophthalmology practice faced $151,695 in coding-related denials due to modifier errors, incorrect CPT/ICD pairings, and NDC discrepancies. MBW RCM corrected the coding issues, appealed denied claims, and helped the practice recover significant revenue.
Ophthalmology Billing: Coding for Cataracts, Glaucoma and In-Office Procedures
Ophthalmology billing requires precision and compliance. This guide simplifies coding for cataracts, glaucoma, and in-office procedures—helping practices avoid denials and increase reimbursements.