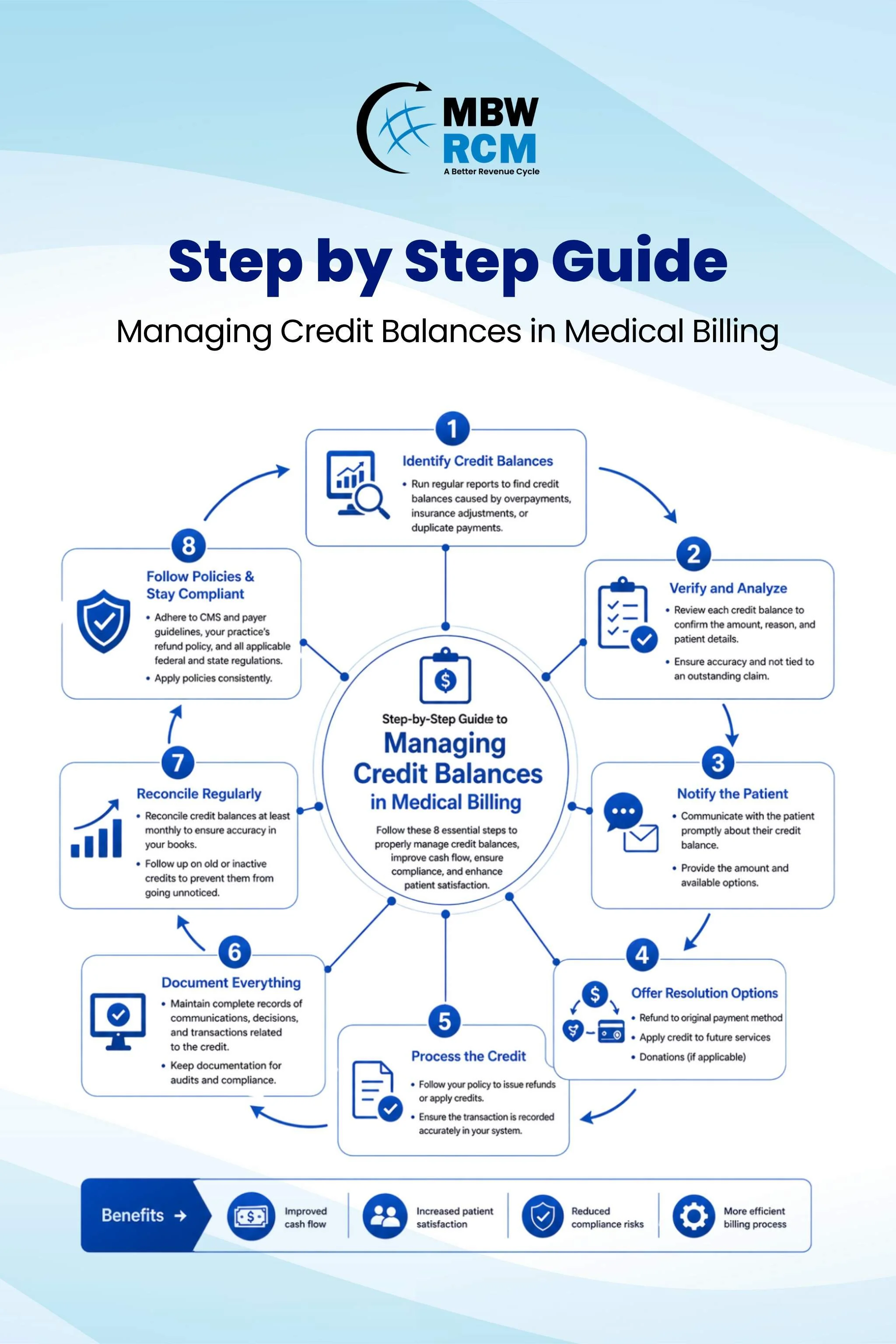
8 Step Guide to Credit Balance Medical Billing Service in RCM
Overpayments and unresolved credits can quietly impact revenue and increase compliance risk in RCM. A reliable credit balance medical billing service in RCM helps healthcare organizations identify, validate, and resolve these balances efficiently across patient and insurance accounts.
From AR identification to reconciliation, adjustments, refunds, and audit documentation, a structured workflow ensures every credit is tracked and cleared correctly. By addressing ERA/EOB mismatches, duplicate payments, and posting errors, this process helps reduce financial leakage and keep the revenue cycle on track.
This guide breaks down 8 practical steps to streamline credit balance handling and improve overall efficiency.
Table of Contents
Step 1: Generate System-Level Credit Balance Report
Credit Balance Management in Medical Billing begins with extracting a structured exception report from the Practice Management (PM) or billing system. This report is the foundation of the entire reconciliation process and is typically run daily or weekly in high-volume RCM environments.
Extract negative balance accounts from AR module
Segment insurance vs patient responsibility credits
Include claim ID, DOS, payer, CPT codes, and payment posting history
Filter aging buckets (0–30, 31–60, 61–90, 90+ days)
In large-scale RCM operations, reports often show 3–7% of total AR in credit status, especially when ERA and EOB posting errors in RCM are not tightly controlled.
Step 2: Segregate Credit Accounts by Payer Responsibility
A structured Credit Balance Process in Medical Billing requires classification of credits by financial ownership before any resolution action.
Primary payer overpayments (Medicare, Medicaid, Commercial)
Secondary coordination credits (COB-related discrepancies)
Patient overpayments from co-pay/deductible duplication
Mixed responsibility accounts requiring split adjustments
Proper segregation reduces processing errors by nearly 25–30% in high-volume billing environments, improving workflow efficiency in Credit Balance Management in Medical Billing.
Step 3: Reconcile Payments with ERA/EOB Transaction Data
A core function of Credit Balance Management in Medical Billing is validating whether payments recorded in the system match payer remittance details.
Match posted payments with ERA (835 files) line-by-line to ensure accurate claim-level posting
Cross-check EOB details with claim adjudication to confirm correct payment interpretation
Verify differences between allowed amount, contractual adjustment, and actual paid amount
Identify duplicate payments, posting mistakes, or missing adjustment codes
ERA and EOB mismatches are one of the main operational reasons for avoidable credit balances, making reconciliation a critical control point in the process.
Step 4: Perform Claim-Level Root Cause Analysis
This step identifies the exact operational or payer-level issue causing the credit balance.
Duplicate claim submission or payment duplication
Incorrect CPT/modifier usage leading to overpayment
COB misalignment between primary and secondary payer
Posting mismatches due to manual entry errors
Frequent ERA and EOB posting errors in RCM are a major driver of unresolved credits, especially in multi-payer claims. A strong credit balance medical billing service in RCM helps reduce recurring issues by identifying system-level gaps at the claim level.
Step 5: Conduct AR Cross-Check Before Resolution
Before initiating any refund or adjustment, a full AR cross-check is performed within the patient account.
Identify open unpaid claims within same patient account
Evaluate eligibility for internal offset adjustments
Check payer recoupment rules and contractual obligations
Validate overlapping service dates and claim linkage
In optimized RCM systems, this step alone reduces unnecessary refunds by 15–20%, improving overall Credit Balance Management in Medical Billing efficiency.
Step 6: Execute Credit Resolution (Adjustment / Transfer / Refund Decision)
At this stage, the resolution path is finalized based on validated findings.
Internal transfer of credit to outstanding AR balances
Contractual adjustment postings using correct adjustment codes
Refund initiation for validated overpayment scenarios
Reclassification of unresolved credits for secondary review
A well-structured Credit Balance Process in Medical Billing ensures that over 70% of credits are resolved internally without refund issuance, improving cash retention and reducing administrative burden. Turn credit balances into revenue opportunities. Make it structured. Be intentional about everything from identifying overpayments to reconciliation and refunds. You get the idea—optimize every step of your RCM workflow.
Step 7: Process Refunds According to Payer Compliance Rules
Refund processing is executed only after full validation and compliance verification.
Follow payer-specific refund workflows (CMS, commercial portals, paper submissions)
Attach supporting documentation (ERA/EOB, claim ID, reason codes)
Issue patient refunds via original payment channel (card, check, EFT)
Track refund turnaround time (typically 15–45 days depending on payer)
Failure in compliance handling increases healthcare credit balance risk in RCM, leading to audit exposure and payer penalties. Strong processes ensure regulatory adherence at every refund stage.
Step 8: Post Resolution, Update AR System & Maintain Credit Balance Audit Log
Final step ensures documentation, traceability, and continuous monitoring.
Post final adjustment/refund entries with correct financial codes
Update claim status in billing system (resolved, pending, escalated)
Maintain centralized credit balance log with aging and resolution type
Perform monthly audit review to identify systemic trends
Continuous tracking helps Improve Credit Balance in Healthcare by identifying recurring operational gaps and preventing future accumulation. Strong Credit Balance Management in Medical Billing relies heavily on audit-driven optimization.
Credit balance prioritization in RCM is used to determine the order of resolving overpayments based on financial impact, aging, and payer risk. A structured approach helps reduce backlog and improve accuracy in financial reconciliation.
How to Prioritize Credit Balances for Faster Resolution
Credit balance prioritization in RCM is used to determine the order of resolving overpayments based on financial impact, aging, and payer risk. A structured approach helps reduce backlog and improve accuracy in financial reconciliation.
Sort by Net Credit Value at Claim and Line Level
Claims are arranged based on total credit amount, focusing first on high-value overpayments. Multi-line claims are reviewed at CPT/service-line level to identify the highest contributing amounts. Larger financial credits are handled earlier to reduce exposure.
Separate System Posting Errors from True Overpayments
Credits are classified into posting errors and actual payer overpayments. ERA mismatches, EOB interpretation errors, duplicate postings, and missing adjustment codes are identified and corrected first to prevent repeated credit generation and AR inconsistencies.
Apply Aging-Based Escalation Rules
Credits are managed based on how long they remain unresolved. 0–30 days follow normal workflow, 31–60 days require validation, and 60+ days are escalated for urgent resolution due to higher audit and recovery risk.
Focus on Credits Linked to Active or Open Claims
Accounts with ongoing activity such as partial payments, COB involvement, or claim reprocessing are addressed earlier to ensure accurate closure and prevent downstream financial adjustments.
Handle Payer-Sensitive and Compliance Cases First
Government payer credits like Medicare and Medicaid, along with audit-flagged or time-bound refunds, are processed on priority to meet regulatory timelines and reduce compliance risk.
Streamline Credit Balance Workflows and Reduce Revenue Leakage
Unresolved credits and overpayments can slow down RCM performance and increase compliance risk. Our Credit Balances Services help healthcare organizations identify aging balances, resolve overpayments, and improve reconciliation workflows for better financial control.
👉 Connect with RCM SpecialistsConclusion:
In medical billing RCM, effective credit balance management directly impacts AR accuracy, cash flow clarity, and compliance readiness. A structured approach ensures that overpayments, ERA/EOB mismatches, and posting errors are identified and resolved on time, preventing unnecessary delays and financial discrepancies.
To improve operational efficiency and maintain clean financial records, outsource credit balance services to a reliable RCM partner.
For better control over credit balance workflows and faster resolution, contact us today.
FAQs on Credit Balance Medical Billing Services
Get Your Free Practice Audit
Apply a structured approach to credit balance medical billing service in RCM with a comprehensive review of your workflows. Our team assesses credit balance reports, ERA–EOB reconciliation, claim validation, posting processes, and refund timelines to identify gaps contributing to aging credits and delays.
Submit the form to connect with our specialists and learn how our Credit Balances Services can support backlog reduction and strengthen control across your revenue cycle.