Credit Balance Process in Medical Billing Explained: How to Fix Backlogs at Scale
The Credit Balance Process in Medical Billing, to begin with, fixes backlogs at scale by using structured workflows, payer validation, and system-driven identification; accordingly, teams detect overpayments early and close accounts within defined timelines.
In most RCM operations, credit balances build due to posting errors, duplicate payments, and delays in reconciliation; therefore, backlog can exceed 5% of total AR if not managed. This guide will help you understand the step-by-step credit balance process and how to fix backlog at scale.
Table of Contents
Step-by-Step Credit Balance Process in Medical Billing
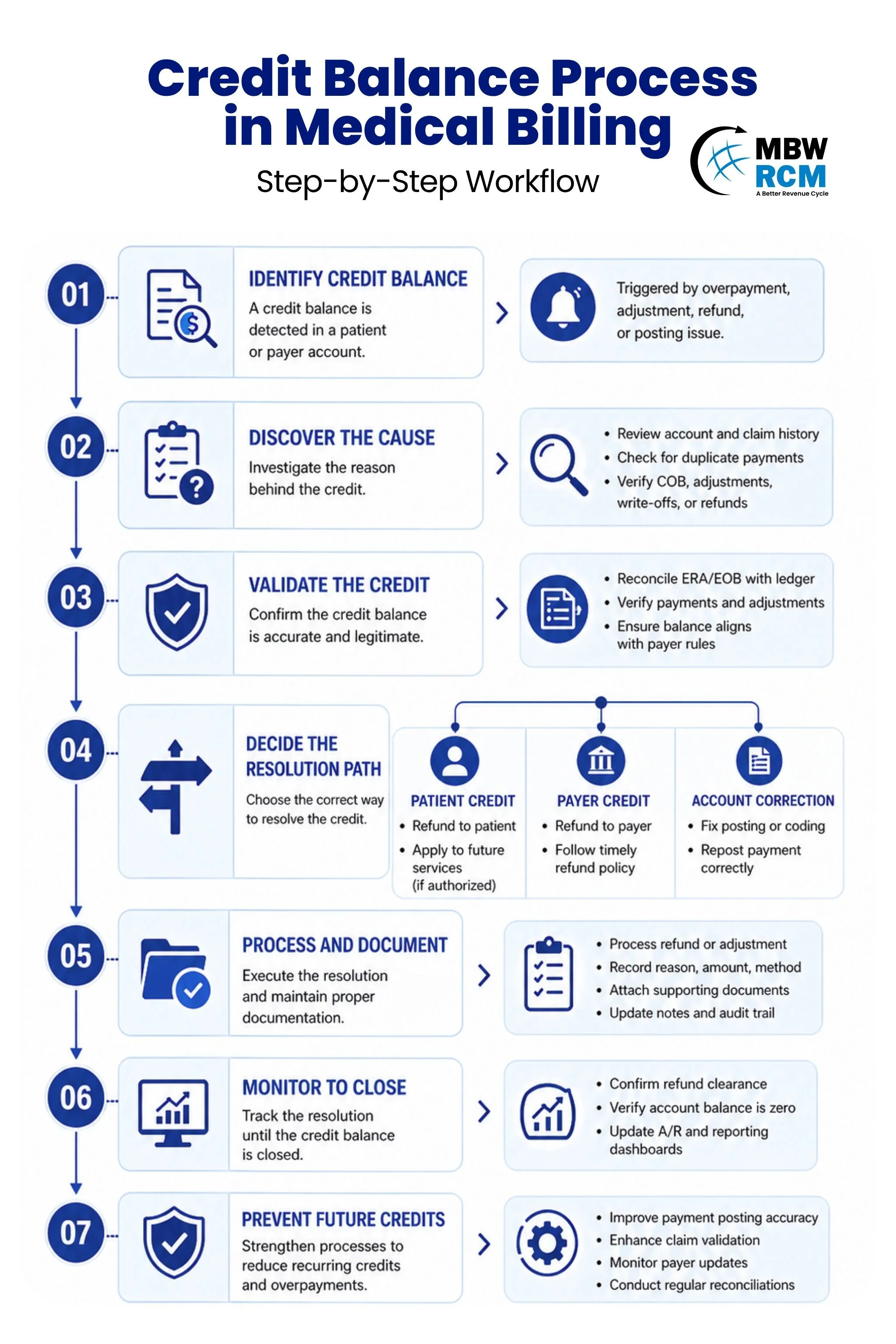
The Credit Balance Process in Medical Billing starts when a patient account shows a negative balance and ends after validation, correction, refund, documentation, and closure.
Credit Balance Identification
First, the system scans ledgers, ERA files, and payment batches to flag negative balances caused by duplicate payments, overpayments, or posting errors.
Account Worklist Creation
Next, identified credits are grouped into worklists based on payer, aging, dollar value, and account type to streamline processing.
Payment and Adjustment Review
Then, analysts review all payments, adjustments, write-offs, and reversals to confirm whether the credit is valid or caused by a posting issue.
ERA, EOB, and Ledger Reconciliation
After that, ERA and EOB data are matched with the ledger to detect hidden gaps in ERA, EOB & ledger posting such as misapplied payments.
Payer Responsibility Validation
Next, payer order and liability are verified using COB details, allowed amounts, and patient responsibility to confirm refund ownership.
Root Cause Classification
Then, the credit is tagged with a root cause such as duplicate payment, overpayment, COB error, or incorrect adjustment.
Refund or Adjustment Decision
Next, the team decides whether to issue a refund, post an adjustment, transfer the balance, or offset against future payments.
Approval and Documentation
Afterward, refund requests are submitted with supporting documents and approved based on payer rules and internal policies.
Refund Processing or Account Correction
Then, refunds are issued or corrections are posted in the system to clear the balance.
Final Account Closure
Finally, the account is rechecked, documented, and closed to complete the cycle and prevent backlog recurrence.
Fix Credit Balance Backlogs in Healthcare Billing at Scale
The Credit Balance Process in Medical Billing, when backlog exceeds thresholds, requires a scale-driven model; accordingly, teams align automation, payer segmentation, and reconciliation to reduce aging credits. In large RCM environments, credits can exceed 5% of AR, with 20%+ in 90+ days, increasing audit exposure.
1. Automation Scale: System-Driven Credit Processing
At the automation level, rule-based tasks are handled through system logic; therefore, manual intervention is reduced across identification, validation, and reconciliation.
Auto-flag credit balances during ERA posting
Trigger work queues based on payer, aging, and value
Use bots/scripts for bulk adjustments and refunds
Apply validation checks for duplicate payments and posting errors
Automation reduces manual workload by 40–60% and speeds up resolution turnaround.
2. Volume Scale: High-Throughput Credit Identification
At the volume level, systems must process thousands of accounts daily; therefore, rule-based engines are configured to scan ERA transaction files, adjustment codes, and ledger entries in real time.
Auto-detect duplicate payments using CARC/RARC codes
Flag negative balances during batch posting cycles
Process 5,000–15,000+ accounts/day in enterprise systems
This reduces manual identification dependency and prevents backlog accumulation at the intake stage.
2. Aging Scale: Time-Based Backlog Control
At the aging level, credits are segmented into defined buckets; consequently, resolution workflows are triggered based on time sensitivity.
Maintaining >90 day credits below 10% is a standard benchmark to control credit balance risks in RCM.
3. Dollar Value Scale: Financial Impact Prioritization
At the financial level, the Credit Balance Process in Medical Billing prioritizes accounts based on refund exposure; therefore, high-value credits are resolved within shorter SLAs.
$1000 → resolution within 7–10 days
$100–$1000 → standard workflow queue
<$100 → batch processing with auto-adjustment
This approach reduces liability exposure and accelerates working capital recovery.
4. Payer Scale: Segmentation Based on Reimbursement Rules
At the payer level, credits are segmented by insurance type; accordingly, workflows align with payer-specific refund timelines and compliance rules.
Medicare → strict 30-day refund requirement
Commercial payers → 30–45 day resolution cycle
Medicaid → state-driven timelines and documentation
Assign payer-specific queues
Apply payer contract logic during validation
Track payer-level backlog separately
Payer segmentation reduces processing delays and improves compliance adherence.
5. Complexity Scale: Effort-Based Case Allocation
At the complexity level, credits are classified based on resolution effort; therefore, workload is distributed to appropriate skill levels.
Low complexity → duplicate payments, posting errors
Medium complexity → COB corrections, partial denials
High complexity → multi-payer disputes, appeals
High-complexity credits require 2–3x more processing time, making allocation critical for resolving credit balances efficiently.
6. Workflow Scale: Parallel Queue Execution
At the operational level, sequential workflows are replaced with parallel processing; consequently, backlog reduction accelerates.
Create separate queues for aging, value, and payer
Run concurrent workflows across teams
Use batch processing for low-value credits
Parallel execution improves throughput by 30–40% and reduces dependency bottlenecks.
7. Data Scale: Fixing Posting Gaps and Reconciliation Errors
At the data level, reconciliation controls are enforced between ERA posting and ledger balances; accordingly, hidden gaps in ERA, EOB, and ledger posting are eliminated.
Auto-match ERA payments with ledger entries
Identify unmatched or misapplied transactions
Trigger correction workflows for posting errors
This reduces false credit creation and helps improve credit balance in healthcare systems.
8. Compliance Scale: Audit and Refund Risk Management
At the compliance level, credits are monitored against regulatory timelines; therefore, high-risk accounts are prioritized for resolution.
Track refund timelines (30–60 days depending on payer)
Flag credits exceeding 90 days
Maintain audit logs for all refund transactions
This reduces exposure to penalties and strengthens control over credit balance risks in RCM.
How Leading RCM Experts Clear Credit Balance Backlogs Faster
Leading teams optimize the Credit Balance Process in Medical Billing through data-driven execution; accordingly, they achieve faster turnaround and lower aging.
Execution Model Used by RCM Experts
Daily monitoring of credit aging buckets (0–30, 31–60, 61–90, 90+ days)
Resolution targets set at 7–10 days for high-value credits
Integration of ERA auto-posting with ledger validation to remove mismatches
Continuous tracking of credit balance risks in RCM through audit dashboards
Performance Benchmarks
“Speed in RCM is not about working faster—it’s about removing what slows you down.”
When Should You Outsource Credit Balance Resolution?
Outsourcing is required when credit balances start impacting resolution timelines, compliance tracking, and daily productivity; therefore, outsourcing credit balance services are used to handle overflow and maintain control.
Credit backlog crosses 8–10% of total AR or credits remain unresolved beyond 90 days, creating audit exposure and delays in resolving credit balances
High-volume workload, payer-specific refund rules, and limited internal bandwidth slow down execution; accordingly, outsourcing credit balance services apply structured workflows and automation to clear backlog within 60–90 days
Fix Credit Balance Backlogs and Improve Resolution Efficiency
Credit balance backlogs can lead to audit exposure, delayed refunds, and operational delays across RCM workflows. Our Credit Balances Services help identify overpayments, resolve aging credits, and streamline reconciliation to improve overall performance.
👉 Request a Free Practice AuditConclusion:
Clearing credit balance backlog at scale requires a structured and consistent approach across identification, validation, reconciliation, and resolution. When workflows are aligned with payer requirements and supported by accurate data checks, teams can reduce aging credits, improve turnaround time, and maintain better control over credit balance risks.
If backlog continues to impact performance or compliance timelines, a more structured execution model is required. Contact us to streamline your credit balance workflow and address backlog at scale with a focused, process-driven approach.
FAQs on Credit Balance Process in Medical Billing
Unlock Faster Credit Balance Resolution — Get a Free Practice Audit
Identify gaps in your credit balance workflow with a detailed review of your current RCM processes. Our team analyzes credit balance reports, ERA–EOB reconciliation, ledger posting, refund timelines, and payer-specific rules to uncover issues that lead to aging credits, backlog buildup, and audit exposure.
Fill out the form to connect with our specialists and learn how our Credit Balances Services can help resolve overpayments, reduce backlog, and improve control across your revenue cycle.